The 4 phases of cardiac rehabilitation describe the broad stages people move through after a heart event, diagnosis or procedure, from the early hospital stage through to long term exercise and ongoing support. If you want the wider picture first, see our main page, Cardiac Rehabilitation In The UK.
Phases 1 to 3 are usually the more time limited parts of recovery, with each stage helping a person move towards greater stability, confidence and activity as appropriate. Phase 4 is different. It is the longer term stage of cardiac rehabilitation, where the focus shifts towards maintaining progress, staying active and continuing with safe, structured exercise over time. This page is here to map the 4 phases of cardiac rehabilitation clearly, so you can see where each stage fits and follow through to the more detailed phase pages where needed.

Why The Phases Matter
A lot of people hear about the 4 phases of cardiac rehabilitation without being fully sure what they mean in real life. The phase model is useful because it gives recovery a clearer shape. Rather than everything feeling vague after diagnosis, discharge or rehab, it helps you see where you are, what that stage is generally for, and what kind of support may be most relevant next.
That does not mean every person moves through the 4 phases of cardiac rehabilitation in exactly the same way. Recovery can look slightly different depending on the heart condition, the treatment received, and the support available locally. Still, the phase structure gives people a practical map. It helps make sense of the journey from acute care through to long term confidence, routine and safer ongoing activity.
What is Phase 1 of Cardiac Rehabilitation?
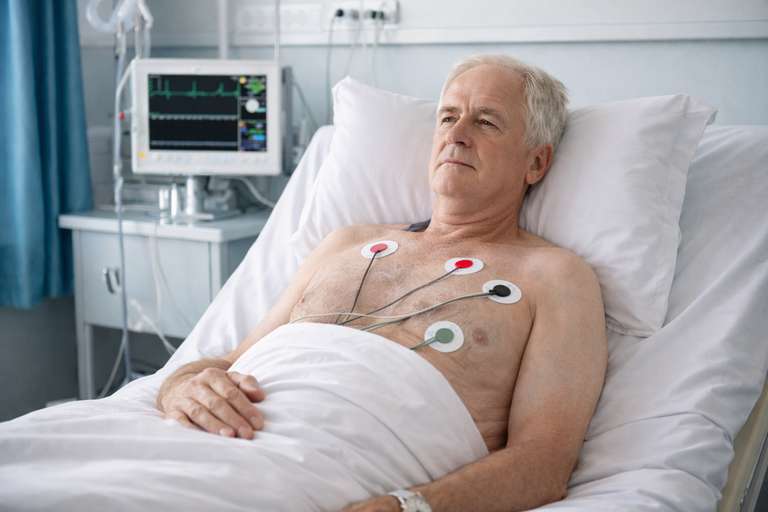
Phase 1 of cardiac rehabilitation is the earliest stage of recovery, usually beginning in hospital after a heart event, diagnosis or procedure. This is the acute stage, when the immediate priority is helping the person become medically stable and preparing them for the next part of recovery.
At this point, people often need reassurance, clear information, and time. It can feel frustrating because so much is out of your hands, but Phase 1 of cardiac rehabilitation is not about pushing on quickly. It is about creating the safest possible starting point for what comes next. If you want a fuller explanation of this stage, read more about Phase 1 hospital care.
What is Phase 2 of Cardiac Rehabilitation?

Phase 2 of cardiac rehabilitation usually begins once a person has left hospital and is continuing recovery at home. It is the early outpatient stage, when the immediate crisis has passed but confidence, routine and day to day recovery still need careful support.
At this stage, people often need practical guidance, reassurance and a sensible plan for rebuilding activity without rushing. Phase 2 of cardiac rehabilitation is usually about recovering at home, getting used to everyday movement again, and knowing where to turn with questions as confidence starts to return. For a fuller explanation of this stage, read more about Phase 2 outpatient care.
What is Phase 3 of Cardiac Rehabilitation?
Phase 3 of cardiac rehabilitation is the more structured stage where exercise, education and support are brought together in a formal rehab programme. For many people, this is the point where recovery starts to feel more active and purposeful, rather than just cautious.
At this stage, people usually need guidance, reassurance and a safe way to rebuild confidence in their body. Phase 3 of cardiac rehabilitation helps people return to activity with more structure, while also learning more about their condition and what supports long term recovery. If you want the fuller detail, read more about Phase 3 exercise and education.



What is Phase 4 of Cardiac Rehabilitation?
Phase 4 of cardiac rehabilitation is the long term stage of recovery, where the aim is to maintain progress, stay active and keep building confidence over time. Within the 4 phases of cardiac rehabilitation, this is the stage that helps people turn structured exercise into an ongoing part of life rather than something temporary.
Unlike the earlier stages, Phase 4 of cardiac rehabilitation does not really have a fixed end point. It is there to support the long term benefits of regular movement, sensible progression and continued confidence after a heart event or diagnosis. For many people, this is where the 4 phases of cardiac rehabilitation start to feel less like recovery in the narrow sense and more like a sustainable way of looking after both physical and mental wellbeing.
The Cardiac Lauren approach to Phase 4 of cardiac rehabilitation is built around making that continuation feel accessible and realistic. Classes are designed so people can exercise at home without needing a gym or lots of equipment, which makes it easier to stay consistent. There is also a range of options to suit different confidence levels, abilities and energy levels, so people can keep engaging with exercise in a way that feels manageable.



Some people feel anxious about exercising more independently at this stage, which is understandable. Phase 4 of cardiac rehabilitation is not about pushing recklessly. It is about continuing in a structured and sensible way. Many people use RPE, the Rating of Perceived Exertion, as one of the tools that helps them judge effort, but the main aim here is long term consistency, not overthinking every session.
Done well, Phase 4 of cardiac rehabilitation can become a sustainable part of everyday life, helping people feel fitter, stronger and more confident in what their body can do. It is the stage within the 4 phases of cardiac rehabilitation where ongoing support, routine and community can make the difference between stopping after formal rehab and continuing to move forwards.
Do The 4 Phases Of Cardiac Rehabilitation Always Happen In Order?
The 4 phases of cardiac rehabilitation are a useful framework, but real recovery does not always feel neat or perfectly sequential. Some people move through the phases quite clearly, while others experience delays, overlaps, or local differences in how support is delivered. That does not mean the model is wrong, it just means the lived experience can be less tidy than the diagram.
What matters most is understanding the purpose of each stage. The 4 phases of cardiac rehabilitation still give you a practical map, even if your own journey has pauses, waiting periods or small detours along the way. The phase model is there to guide recovery, not to make you feel you are somehow doing it wrong if your path looks slightly different.
What Happens After The 4 Phases Of Cardiac Rehabilitation?
In one sense, nothing happens after the 4 phases of cardiac rehabilitation, because Phase 4 is the ongoing stage. It is the part of the pathway where people keep building on what they have learned and try to make exercise, confidence and sensible self management part of ordinary life. That is why Phase 4 matters so much, because it is where recovery becomes something you continue to live, not just something you once completed.
For many people, the real challenge after the 4 phases of cardiac rehabilitation is not knowing what to do next, but keeping enough structure in place to carry on. That is where ongoing support, community and routine can make a real difference. Rather than stopping when formal rehab ends, the aim is to keep moving forwards in a way that feels safe, sustainable and realistic.

